Menu
Close
Back
Welcome to
Together is a new resource for anyone affected by pediatric cancer - patients and their parents, family members, and friends.
Learn MoreParenteral nutrition (PN) is intravenous (IV) nutrition given through a catheter placed in a vein. It is used when the patient is not able to get all the nutrients they need by mouth or by enteral (tube) feeding. Parenteral nutrition is given as a liquid solution directly into the blood stream. It provides the calories and nutrients that a patient needs.
Parenteral nutrition may be used for partial or complete nutrition support. Complete nutrition support is known as total parenteral nutrition (TPN).
Different types of IV catheters can be used for parenteral nutrition. These include:
When possible, it is best to provide nutrition by mouth or tube feeding. These methods allow digestion to occur in a more natural way. In children with cancer, this is not always possible. Parenteral nutrition may be needed when:
The PN solution is prepared in a pharmacy. It is a sterile liquid that contains a mixture of key nutrients. The formula is customized to meet a patient’s specific nutrition needs based on factors such as age, weight, and health.
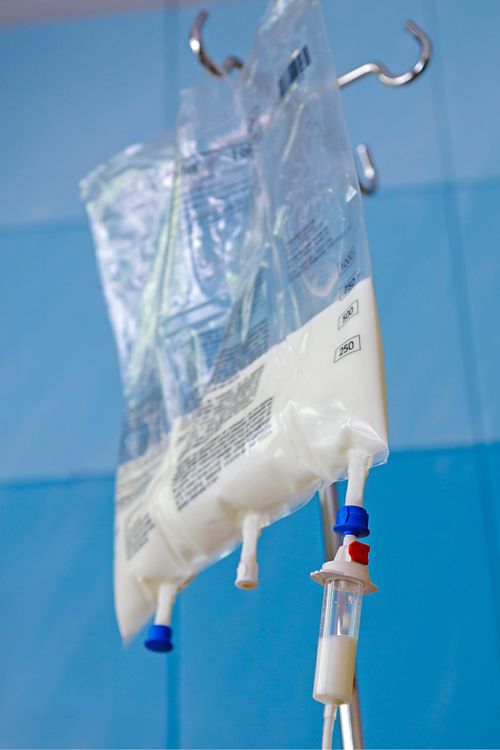
The parenteral nutrition solution is a sterile liquid that contains a mixture of key nutrients, customized to meet a patient’s specific nutrition needs.
Carbohydrates, proteins, and fats are 3 main nutrients that provide calories for energy and are used in different body functions.
PN also provides:
Parenteral nutrition is usually started in the hospital. A doctor, pharmacist, and registered dietitian work together to determine how many calories and other nutrients the patient needs each day. Blood tests are used to monitor response to PN. The PN mixture is adjusted as needed.
Usually, patients receive one bag of PN solution per day. PN comes in 2-in-1 (dextrose and amino acids) and 3-in-1 (dextrose, amino acids, and lipids) solutions. If the solution contains lipids, the bag will have separate chambers. The nutrients need to be mixed together by removing the dividing strip and gently kneading right before infusion. The solution is given by connecting the bag to the patient’s IV or central line and using an infusion pump. The pump is set to give the solution on a specific schedule.
Continuous PN is given all the time. This method is used when PN is first started. This allows the body to adjust to make sure that nutrition needs are met.
Cycled PN is given over specific time periods for less than 24 hours in a day. The pump is set to give PN on a cycle for a set number of hours, such as 20, 16, or 12 hours. As the cycle time is decreased, the rate of infusion is increased so that the overall PN is constant.
Benefits of cycled PN:
Most patients have cycled PN overnight to allow a few hours of normal activity during the day. Depending on the device, the infusion pump can be worn in a backpack to allow more freedom of movement during PN infusion.
Careful monitoring is needed to ensure proper nutrition and to prevent serious side effects. Many problems that occur with PN can be managed by adjusting the PN formula or schedule. It is also important to take good care of the central venous catheter to prevent infection. Proper hand washing and using aseptic technique when connecting and disconnecting PN are important.
Possible complications of PN include abnormal glucose levels, liver problems, changes in electrolytes, vitamin or mineral deficiencies, and catheter-related problems including infection, thrombosis, or blockage. PN may also change the way some medications work.
A common problem with PN is hyperglycemia, or high blood sugar. Hyperglycemia can occur when the body cannot use glucose well enough and blood glucose levels rise above normal. This may happen when PN is given too quickly so the body cannot process the sugar. It can also be caused by an infection or a medicine such as a steroid. Symptoms of hyperglycemia include headache, feeling thirsty, weak, or nausea. To prevent problems such as hyperglycemia, the amount of carbohydrate (dextrose) in PN is increased gradually over several days. Hypoglycemia, or low blood sugar, is less common but can occur if PN is stopped suddenly.
Monitoring during PN may include tests to measure:
Patients can receive PN at home. Before going home, family caregivers will be taught how to:
—
Reviewed: June 2018