Menu
Close
Back
Welcome to
Together is a new resource for anyone affected by pediatric cancer - patients and their parents, family members, and friends.
Learn MoreTube feeding, or enteral nutrition, provides nutrition in liquid or formula form through a hollow tube placed into the stomach or intestine. Some medicines may also be given through the feeding tube.
Dietitians are experts in food and nutrition. Your dietitian will work with you and your doctor to plan tube feedings to make sure your child’s nutrition needs are met. You will learn how to mix formula, give feedings, and take care of the feeding tube.
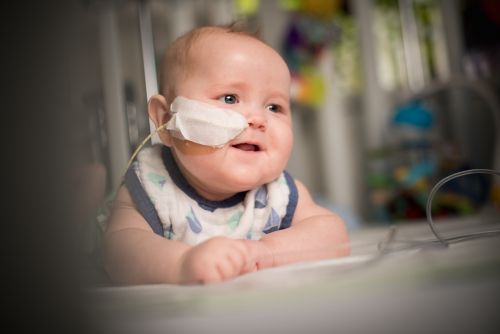
Some children need a feeding tube for nutrition support during cancer or other illness.
There are generally two ways feeding tubes are placed:
The most common feeding tubes include nasogastric tubes (NG tubes) and gastrostomy tubes (G tubes). However, there are several types of feeding tubes based on how and where they are placed in the digestive system.
Learn more about types of feeding tubes and how they are placed.
During illness and recovery, some patients may not be able to get all the calories and nutrients they need by mouth. This is no one’s fault. It is important to help children understand that nutrition support (enteral nutrition) is not a punishment. Most children adapt well to having a feeding tube.
Make sure your child doesn’t touch or pull on the tube. Follow instructions for skin care around the tube site to prevent irritation or infection.

A G tube, or gastrostomy tube is a type of feeding tube used for enteral nutrition.

The G tube is inserted through the abdominal wall into the stomach. On the outside of the body, patients have a long tube or a button tube.
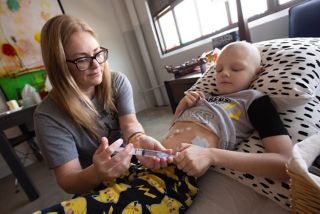
For children with cancer, feeding tubes are often used to supplement what the patient can eat by mouth.

Children may go home with a feeding tube. The care team will make sure that families know how to give feedings and care for the feeding tube.

The stoma should not be painful once healed. Children should be able to do most regular activities.
The most common side effects of tube feeding are nausea, vomiting, stomach cramps, diarrhea, constipation, and bloating.
Other possible side effects may include:
Most side effects can be prevented by following instructions for care and feeding.
For many patients, a feeding tube is often used to supplement what the child is able to eat by mouth. Other patients may get all nutrients from a feeding tube.
A dietitian or nutritionist will make sure that your child’s specific nutrition needs are met. Your child’s nutrition formula will be prescribed based on:
Many patients can be fed with standard formulas. For infants, breast milk is often preferred. Other children need special formulas for medical conditions such as allergies, diabetes, or digestive problems.
It is important to work closely with your nutrition professional. Nutrition needs may change based on health factors and side effects such as vomiting or diarrhea.
There are 3 main ways to give tube feedings: bolus feeding, continuous feeding, and gravity feeding.
Bolus feeding – In bolus feeding, large doses of formula are given several times a day through the feeding tube. This is most like a normal eating routine.
Continuous feeding – In continuous feeding, an electronic pump is used to give small amounts of formula for long periods of time, up to 24 hours a day. Some children may need continuous feeds to help reduce nausea and vomiting.
Gravity feeding – In gravity feeding, a feeding bag is placed on an IV pole. A set amount of formula drips through the tube at a slow rate. The amount of time varies by patient.
Your child may go home with a feeding tube. The care team will make sure that you know how to give feedings and care for the feeding tube. Watch for problems such as:
Eating involves the mouth and face. It is important to help your child use their mouth and lips and stay aware of the movement and feeling of their mouth and face. Touching your child’s lips, mouth, or gums during feedings will make it easier for your child to go back to eating by mouth when the feeding tube comes out.
A speech language pathologist can give you other suggestions for helping your child remember that feeding involves the mouth and face. Your therapist may recommend oral stimulation tools or activities to help your child develop or maintain the skills needed for feeding.
—
Reviewed: September 2022