St. Jude Family of Websites
Explore our cutting edge research, world-class patient care, career opportunities and more.
St. Jude Children's Research Hospital Home

- Fundraising
St. Jude Family of Websites
Explore our cutting edge research, world-class patient care, career opportunities and more.
St. Jude Children's Research Hospital Home

- Fundraising
Elaine Tuomanen Lab
Investigating the molecular pathogenesis of Streptococcus pneumoniae and developing new therapeutic approaches
About the Tuomanen Lab
Streptococcus pneumoniae infection causes more death in children that any other bacteria. It traffics from one place to another within the body causing a host of diseases. Our laboratory leads an expansive and innovative research portfolio to uncover the molecular mechanisms of infection. We are also translating that understanding into potential powerful therapeutics.

Our research summary
The major focus of the lab is the molecular pathogenesis of invasion and inflammation induced by Streptococcus pneumoniae, a leading worldwide bacterial threat. Our research leverages unique strengths in gram-positive bacterial molecular biology and genomics, in vitro models of gram-positive bacterial interactions with human cells, and animal models of disease. The breadth of our research is unusual in the field of microbial pathogenesis and reflects a strong commitment to translating our molecular understanding into the therapeutic setting, including through the use of antibiotics and vaccines.
One area of research in our laboratory focuses on meningitis and understanding the elements of pneumococcus that are bioactive when these bacteria reach the brain. The classical biological response to infection is inflammation that leads to neuronal cell death and we have developed strategies to decrease brain damage. Conversely, exposure to pneumococcus in a fetal environment results in increased neuronal proliferation. We are investigating how components of S. pneumoniae, recognized by the immune system, switch signals from inflammation to neurodevelopment.
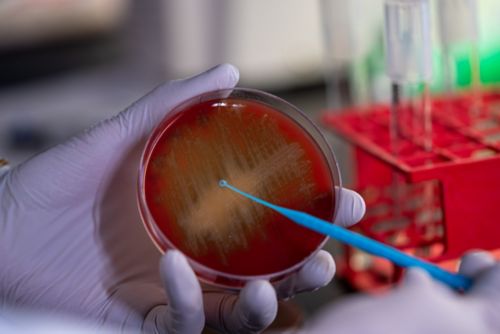
Our laboratory is also invested in vaccine development. In order to build a vaccine that protects against pneumonia, sepsis, meningitis, earaches and other conditions, a common set of components needs to be identified between the different bacteria strains. Our laboratory has created a multi-component, protein-based vaccine – the first of its kind for pneumococcal infection. We have completed preclinical development and this vaccine will soon enter clinical trials to test whether it is protective against the different forms of pneumococcal infection.
In addition, we are investigating the earliest steps in how bacteria develop antibiotic resistance, a step known as tolerance. S. pneumoniae bacteria have a specific response when treated with an antibiotic like penicillin - that is to ‘blow themselves up’. In the process they release hundreds of different molecules that are bioactive and cause inflammatory responses at the site of an infection. We are investigating how to regulate this explosive process and gaining a better understanding of how bacteria have developed means of evading therapeutic intervention.
The work in our laboratory leverages the unique insights and expertise of both MDs and PhDs and involves genetics, microbiology, animal model systems, sequencing, flow cytometry, structural biology, chemical biology, and various imaging techniques.

Selected Publications
About Elaine I. Tuomanen
Dr. Elaine I. Tuomanen earned her BS and MD from McGill University in Montreal before completing pediatric infectious diseases fellowship training at the University of Virginia and the Rockefeller University. She then served as a faculty member and the head of the Laboratory of Molecular Infectious Diseases at Rockefeller University before joining St. Jude in 1997. Dr. Tuomanen leads an innovative research program that focuses on the pathogenesis of Streptococcus pneumoniae and how that bacterium invades the human host and leads to disease.

Meet the team
The Tuomanen Lab team proudly mixes the worlds of MDs and PhDs to take full advantage of designing new therapeutics from both ends of the discovery spectrum.
-
View Details
Beth Mann, BS
Sr. Scientist
Contact us
Elaine I. Tuomanen, MD
Member, St. Jude Faculty
Host-Microbe Interactions
Room DT2058F, MS221
St. Jude Children's Research Hospital

Memphis, TN, 38105-3678 USA GET DIRECTIONS
