St. Jude Family of Websites
Explore our cutting edge research, world-class patient care, career opportunities and more.
St. Jude Children's Research Hospital Home

- Fundraising
St. Jude Family of Websites
Explore our cutting edge research, world-class patient care, career opportunities and more.
St. Jude Children's Research Hospital Home

- Fundraising
Accelerating Discovery
St. Jude was founded on big dreams and a trailblazing spirit. From the beginning, the premise was daring. In 1962, when the hospital opened, a mere 20% of those with pediatric cancer survived. Children with sickle cell disease lived from pain crisis to pain crisis.
The hospital has grown exponentially since its opening, but the urgency of the work remains the same. Scroll through the timeline below to see a few of the milestones in our journey to advance cures and means of prevention for pediatric catastrophic diseases through research and treatment.
1960s
1962

The hospital opens in Memphis, Tennessee, before a crowd of 9,000 people.
St. Jude initiates the Total Therapy approach to acute lymphoblastic leukemia (ALL) treatment. The four-component approach still forms the backbone of ALL treatments today.
1965
1966
A group of St. Jude patients with ALL are successfully taken off therapy, providing evidence that remission can be sustained.
1968
1969
St. Jude partners with Memphis Area Project South (MAP-South) as one of the first sites in the U.S. to participate in a USDA food distribution program, which serves as the prototype for WIC, the federal health and nutrition program for women, infants and children.

1970s
1972
1975
St. Jude becomes the first to identify important subtypes of ALL, including T-cell leukemia. The finding leads to better risk classifications, new research directions and improved treatment.
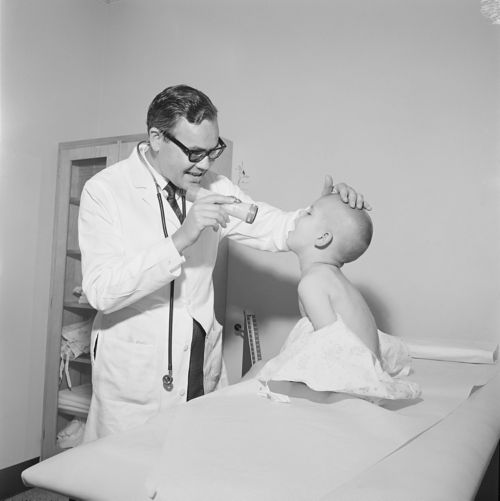
1975

World Health Organization (WHO) designates St. Jude as a Collaborating Center for the study of influenza transmission from animals to humans.
1977
1980s
1983
1984
St. Jude opens the After Completion of Therapy Clinic, which is now the world’s largest long-term follow-up clinic for pediatric cancer patients.
1985
The hospital’s brain tumor program, which opened the previous year, begins accepting patients. St. Jude forms a partnership with Le Bonheur Children’s Hospital, creating one of the largest pediatric surgical brain tumor programs in the country to provide high quality care for patients.
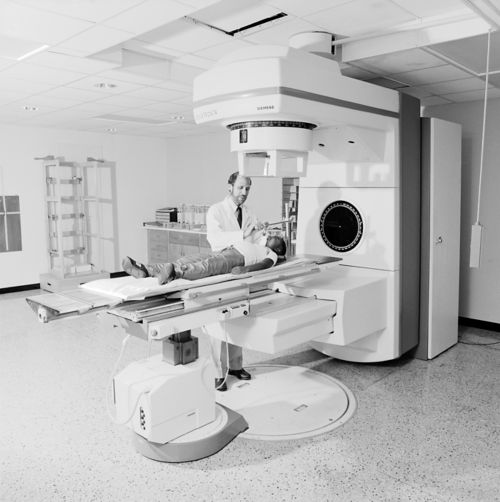
1987
Danny Thomas declares AIDS a catastrophic disease of children, and St. Jude prioritizes HIV/AIDS research with the creation of a new clinical program.
1990s
1991
St. Jude is the first to use gene marking to follow the course of bone marrow transplantation in children.
St. Jude scientists discover that an antimalarial drug can prevent or effectively treat a life-threatening form of pneumonia in patients with AIDS.
1992

St. Jude forms a Pediatric AIDS Clinical Trial Unit with two other Memphis area hospitals.
1993
Arthur Nienhuis, MD, establishes an experimental hematology program with a focus on developing gene therapy for blood disorders.

1994
1995
St. Jude is among the first to incorporate a computer-based, 3-D radiation therapy technique into pediatric brain tumor treatment.
1996
By opening vector production labs, St. Jude becomes one of the few centers in the world with a comprehensive cell and gene therapy program.

Peter Doherty, PhD, St. Jude Immunology chair, is awarded the Nobel Prize for Physiology or Medicine. He and Rolf M. Zinkernage, MD, PhD, of the University of Zurich, share the prize for their earlier pioneering work on identifying the role of T-Cells in fighting virus-infected cells.
1998
1999
2000s
2001
2002
2003
St. Jude becomes the nation’s first pediatric cancer research center to open a Good Manufacturing Practices (GMP) facility to produce vaccines, proteins, gene-based molecules and other biopharmaceuticals.

2004
2005
2006
St. Jude reports a 94% survival rate for patients with ALL, using therapy that does not include radiation.

2007
2008
2009
2010s
2010
2012
The Pediatric Cancer Genome Project announces the largest-ever release of comprehensive human cancer genome data for free access.
2013
The Pediatric Cancer Genome Project identifies drugs that enhance oxidative stress as a possible treatment against rhabdomyosarcoma, the most common pediatric soft-tissue tumor.
2014
The Pediatric Cancer Genome Project offers new leads for improved outcomes in children with high-grade glioma brain tumors.
2015
St. Jude opens the world’s first proton therapy center for children with cancer.
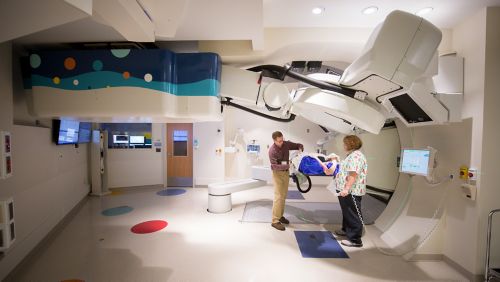
A study from the Pediatric Cancer Genome Project suggests that comprehensive genomic screening may be warranted for all pediatric cancer patients, not just those with family histories of cancer.
2016
St. Jude is named a trial site for an HIV Prevention Trials Network study that compares for pre-exposure prevention of HIV in young men.
2017
2018
St. Jude-led research offers the most comprehensive analysis yet of the genomic alterations that lead to cancer in children and affirms the need for pediatric-specific precision therapies.
2019
St. Jude announces a cure for SCID-XI, commonly known as bubble boy disease. Investigators at St. Jude and UCSF Benioff Children’s Hospital San Francisco use novel treatment that combines gene therapy developed at St. Jude and low-dose chemotherapy with busulfan to restore complete immune function in infants newly diagnosed with SCID-X1.

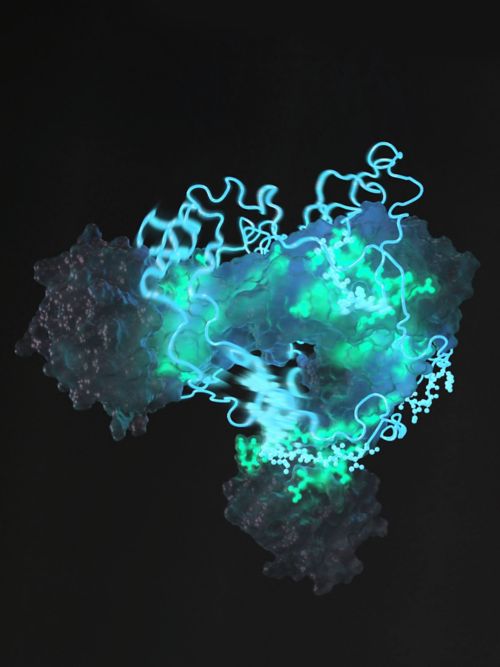
St. Jude acquires the nation’s largest and most powerful nuclear magnetic resonance spectrometer to visualize protein structures that cannot be detected with other technology.
2020s
2020
An international collaboration led by St. Jude shows therapy-induced mutations can drive about 25% of relapsed acute lymphoblastic leukemias.
Scientists develop the Childhood Solid Tumor Network (CSTN) data portal on St. Jude Cloud. The CSTN includes wide-ranging data on 170 patient-derived samples that represent 21 types of childhood solid tumors.
2021
By October 2021, the Global COVID-19 Observatory and Resource Center for Childhood Cancer had tracked 1,775 COVID-19 positive cases from 51 countries. This project provides an unparalleled resource for understanding how the SARS-CoV-2 virus affects children undergoing cancer treatment around the world.
2022
Scientists at St. Jude develop a method that may be able to improve chimeric antigen receptor (CAR) T-cell therapies by identifying the early cells that become the most effective cancer killers.
2023
2024
Using information gathered in a collaborative clinical genomics pipeline, scientists and clinicians at St. Jude identify a BARD1 mutation in a patient with high-risk neuroblastoma and create a targeted treatment protocol that led to complete response, paving the way for other pediatric patients with BARD1 mutations.

2025
Explore more
Learn more about the history of the hospital, our in-depth scientific accomplishments and the profound impact of our research enterprise at the links below.