St. Jude Family of Websites
Explore our cutting edge research, world-class patient care, career opportunities and more.
St. Jude Children's Research Hospital Home

- Fundraising
St. Jude Family of Websites
Explore our cutting edge research, world-class patient care, career opportunities and more.
St. Jude Children's Research Hospital Home

- Fundraising
Molecular diagnostics bring treatment opportunities to infants with brain tumors
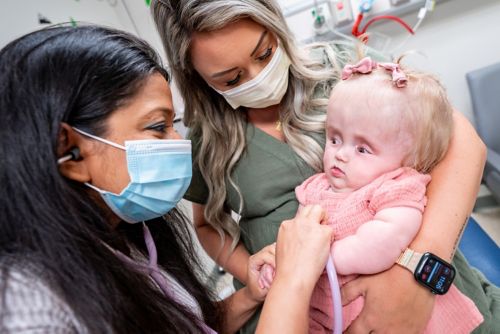
An integrated, molecular diagnosis allows Aditi Bagchi, MD, PhD, to provide a treatment plan for Fletcher Fazenbaker, who reclines in Stevee Fazenbaker’s arms during a checkup.
It had been a long day in the St. Jude Brain Tumor Clinic for one-year-old Fletcher Fazenbaker. After checkups and exams with her doctors, Fletcher’s cheery demeanor faded into restless squirms that ruffled her pale pink dress as she reclined in her mother’s arms. But Stevee and Billy Fazenbaker, Fletcher’s parents, knew what to do. Billy pressed play on his iPhone, and as the melody of “Skidamarink A Dink A Dink” filled the tree-themed walls of Exam Room 4, Fletcher’s lips curled into a gum-filled smile.
When Fletcher first arrived at St. Jude at three months old, her parents did not know what to expect. In November 2022, when the family of three packed their belongings and drove from Maryland to Tennessee, Stevee and Billy Fazenbaker admit their hearts were guarded. In their first few months as new parents, the Fazenbakers experienced what most could not begin to fathom.

Billy and Stevee Fazenbaker pose for a family portrait with their daughter, Fletcher, and their dog, Hank.
Mere days after Fletcher was born with an enlarged head, she was diagnosed with a congenital brain tumor — taking up roughly half her brain — and given a two-week life expectancy. She was sent home on hospice care, and Billy and Stevee were told to cherish their time with their newborn daughter.
But two weeks turned to four, then eight, and Fletcher’s development progressed despite doctors’ grim predictions. By month three, the Fazenbakers watched their daughter take a binky, suck a bottle, breastfeed, kick and cry. But the answer from doctors did not change: Fletcher was to remain on hospice care. A desire for clarity and peace, and a suggestion from a hospice nurse, brought them to St. Jude. The Fazenbakers submitted a second opinion form and received a swift response: could they be in Memphis in two days?
“All we really wanted was another MRI, just to see everything again, to see if anything had changed, just another MRI,” says Stevee Fazenbaker.
When the family arrived at St. Jude, they received so much more.
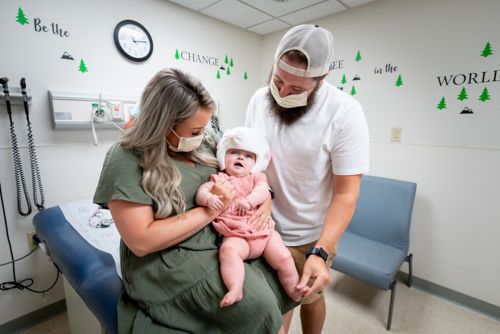
Stevee, Fletcher and Billy Fazenbaker in the St. Jude Brain Tumor Clinic.
A molecular diagnosis for Fletcher
Aditi Bagchi, MD, PhD, Department of Oncology, Division of Neuro-Oncology, is well-versed in this kind of story. When she first viewed Fletcher’s medical files, she was once again confronted with a situation she says breaks her heart.
Bagchi explains that most of these babies are diagnosed at birth when the initial symptom is labor that does not progress because of an enlarged head. When the babies are born, an ultrasound reveals a large tumor that sometimes takes up half the brain, and families are told the tumor is incurable. Most are sent home on hospice care.
“But we sometimes have families reach out with babies up to five months into hospice who say, ‘This baby has a huge tumor, and everyone says it is incurable, but the baby is progressing.’ And we tell them to come to St. Jude,” says Bagchi.

Fletcher Fazenbaker grasps Aditi Bagchi’s, MD, PhD, finger during a checkup at St. Jude.
Once the Fazenbakers arrived at St. Jude, the clarity they sought became a reality. Fletcher quickly received a cranial shunt to relieve pressure from excess fluid in her head, which allowed the medical team to collect a biopsy. Molecular analysis of the tumor revealed what Bagchi suspected all along.
Fletcher’s brain tumor, previously described generically as “congenital,” is an infant-type hemispheric glioma (IHG) — a subtype of high-grade glioma that, up until 2021, did not exist in the World Health Organization’s brain tumor classification guide.
Bagchi spent years studying pediatric high-grade gliomas as co-investigator on a St. Jude Clinical trial called SJYC07. Under the leadership of study principal investigator Amar Gajjar, MD, Department of Oncology, Division of Neuro-Oncology, results from the SJYC07 clinical trial were published in Neuro-Oncology.
Based on what she learned through SJYC07, Bagchi was able to give the Fazenbakers something they thought they would never receive: a diagnosis and treatment plan for Fletcher.
Molecular differences identify targets for treatment
While high-grade gliomas in very young children (younger than three years old) have generally favorable outcomes, a lack of accurate diagnoses and varied treatment approaches have historically made outcomes unpredictable, especially among different pediatric age groups.
Giles Robinson, MD, Department of Oncology, Division of Neuro-Oncology, and co-investigator of SJYC07, explains it was well known that very young children with high-grade gliomas have better outcomes than older children, but no one knew why.
It was only in the past few years that retrospective research conducted by various investigators offered an explanation. Most of the research, which focused on the molecular characteristics of these tumors, revealed a new category of brain tumor: infant-type hemispheric glioma. The diagnosis primarily impacts children under three years of age.
“So, what we thought was a difference of age is actually a molecular difference,” says Bagchi.

Copies of the 2007, 2016 and 2021 World Health Organization’s brain tumor classification guides.
These molecular differences among high-grade gliomas challenged the historical homogenous categorization of this brain tumor. While previous discoveries enhanced the biological understanding of high-grade gliomas, investigators on the SJYC07 trial wanted to know how these molecular differences could lead to targeted treatments.
From 2007 to 2020, 56 children who had been histologically diagnosed (via microscopic examination of tumor samples) and treated for high-grade gliomas at St. Jude were identified. Retrospective and prospective molecular testing (via genome-wide methylation profiling and next-generation genomic sequencing) of the tumor samples, combined with histologic analysis, showed these children with high-grade gliomas could be split into four diagnostic categories: patients with infant-type hemispheric glioma (IHG), high-grade glioma (HGG), low-grade glioma (LGG) and other central nervous system (CNS) tumors. IHG was the most prevalent tumor category and affected the youngest children who commonly had receptor tyrosine kinase gene fusions (ALK, ROS1, NTRK1/2/3, MET).
Identifying the gene fusions provides specific targets for new molecular therapies that shrink the tumor and decrease adverse effects associated with traditional treatments like radiation and chemotherapy. When given prior to surgery, these molecular therapies can help shrink the tumor and increase the likelihood of successful surgical removal. While results from the trial demonstrate favorable survival outcomes for children with IHG and LGG, the investigators call for more exploration of targeted molecular treatments that further reduce adverse effects.
The goal is to not only find a cure but also improve the quality of life.
Combining methods for more accurate brain tumor diagnoses
For investigators, the results from SJYC07 confirm that using one diagnostic method is not enough to develop adequate treatment plans for pediatric high-grade gliomas. Bagchi stresses that just looking at a brain scan does not yield enough information about this type of tumor. “We want to know what kind of high-grade glioma it is,” she says.
The best way to do this? Integrate multiple diagnostic methods. For example, medical teams can use histopathologic classification methods, such as how the tumor looks under the microscope, along with more advanced molecular classification methods, such as genome-wide DNA methylation (to characterize methyl group additions to DNA that dictate gene expression) and next-generation genomic sequencing (to identify how genes are changed or expressed) to analyze and classify the tumor samples comprehensively. The result is an integrated diagnosis with powerful implications for treatment planning.
“By looking at the molecular profiling of these tumors, we decide who needs what treatment. That is the most important thing,” says Bagchi.

Aditi Bagchi, MD, PhD; Jason Chiang, MD, PhD; Sandeep Dhanda, PhD; and Giles Robinson, MD, discuss integrated diagnostic methods for IHG tumors.
Jason Chiang, MD, PhD, Department of Pathology and co-investigator on SJYC07, emphasizes that histology is often insufficient for a pathologist to make an informed diagnosis for high-grade gliomas. For him, analyzing the different aspects of the tumor is of utmost importance because “we know the tumor better. You’re looking at the picture of a person, and you can have a certain impression based on experience, and maybe you are right, but you won’t be one hundred percent right. You want to know all other aspects about that picture,” he says.
Unfortunately, achieving this level of integrated diagnosis requires extensive technological resources and personnel expertise, which is not available everywhere. But Chiang says, “We can educate other pathologists. If you see a tumor in a baby that looks like this, and there is an association with specific marker alterations, then maybe you need to find a place — here, we do it for free — to get this analysis done. Then the patient may have a chance of targeted therapy.”
Bagchi echoes Chiang’s sentiment. “What we have been seeing in the past few years is the fact that IHG is such a curable entity, and that is largely unknown to the general pediatric medical professionals,” says Bagchi. “There is a possibility here for treating these tumors, and we don’t want anyone to write these babies off.”
Data portal helps researchers recognize patterns
As part of the effort to advance knowledge and education about this tumor type, the data from SJYC07 is readily accessible to the clinical and research communities via a data portal.
For Robinson, the hope is to provide an access point where “almost all the cases we’ve seen at St. Jude are mapped out with their different molecular aspects, their different histologic patterns and their different outcomes on therapy. Other researchers can look up our data when they get a similar tumor at their institution and say, ‘Oh, they’ve had seven kids with the same thing. They tried three different treatment methods. And the third one was the best,’” he explains.
Beyond data sharing, the development of the portal provides a tool to translate molecular aspects of a tumor into actionable therapeutic approaches. For Robinson, this translational ability has been a career-defining shift.
Over the years, Robinson has sorted through immense amounts of data from large cohorts of patients to discern what molecular tumor characteristics dictate a particular treatment.

Fletcher Fazenbaker smiles at the camera.
He admits that for years, he put molecular characteristics on spreadsheets to try and sort tumors into different molecular categories. But as technology evolved, bioinformaticians were able to move Robinson’s spreadsheets into a new age.
He explains that bioinformaticians take this molecular information and put it into a visual format that clusters the molecular groups. “From there, it’s all about pattern recognition,” says Robinson.
The data portal developed by St. Jude bioinformaticians enables such pattern recognition. Sandeep Dhanda, PhD, Department of Oncology, is one of the bioinformatics scientists who built this visualization capability. Developing the portal brought a career first for Dhanda, who welcomed the opportunity to work with genomic and methylation data from patients. For Dhanda, work on the portal was driven by the goal of assessing “what kind of data we have and how can we make it more useful for the clinician to make routine decisions.”
The ability to visually assess and recognize patterns in brain tumors advances communication and diagnostic ability across the medical team. Robinson says a tool like the portal enables pathologists like Chiang to group tumor types and recognize patterns across their cell architecture. For physicians, the portal helps translate these patterns into therapy, where it is easy to see outcome patterns across tumor types and treatment approaches.
“What we’re doing is hopefully going to introduce the appearance of what most of these cases look like. A standard picture,” says Robinson.
Targeted therapy helps unlock new milestones
The standard picture that Robinson, Bagchi and their colleagues were able to create from SJYC07’s data led to Fletcher’s integrated diagnosis and subsequent treatment plan, which has allowed Stevee and Billy Fazenbaker to move from “grieving someone who is still alive to celebrating her,” they say.
On July 24, 2023, the Fazenbakers did just that. Amidst all the treatments and checkups, they celebrated an anniversary they never thought they would see: Fletcher’s first birthday.

Fletcher Fazenbaker poses for her one-year photos.
At a rodeo-themed birthday party in her grandparents’ barn in Maryland, Fletcher donned a cowgirl getup, enjoyed her first cupcake — a raspberry-filled vanilla confection — and listened to the harmony of “Happy Birthday” from the dozens of family and friends who gathered to celebrate her. The Fazenbakers will have another anniversary to celebrate in November 2023, when they welcome their second child and become a family of four.
As Fletcher prepares for her new role as big sister, she continues to progress and gain developmental milestones. Stevee says, “One of our biggest goals right now is more head control. That is really going to open up so many new things for her. But we work on rolling, picking things up, shaking things and kicking. She really never stops moving unless she’s sleeping. She’s a very busy girl.”

Fletcher Fazenbaker smiles at the camera after a busy day.

Fletcher, Billy and Stevee Fazenbaker at Fletcher’s rodeo-themed first birthday party.
Learn more
- Learn more about pediatric brain and spinal cord tumors
- Explore the Brain Tumor Program at St. Jude
- Dive into the infant high-grade glioma data from St. Jude
- Discover all neuro-oncology data from St. Jude






