St. Jude Family of Websites
Explore our cutting edge research, world-class patient care, career opportunities and more.
St. Jude Children's Research Hospital Home

- Fundraising
St. Jude Family of Websites
Explore our cutting edge research, world-class patient care, career opportunities and more.
St. Jude Children's Research Hospital Home

- Fundraising
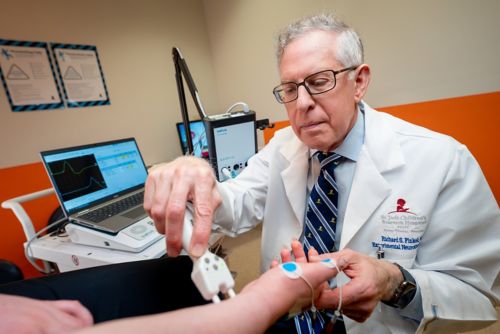
Richard Finkel, MD
Developing transformative, gene-targeted therapies and clinical trial strategies for pediatric neurological diseases.
Overview
The field of pediatric neurology has undergone substantial changes in recent decades in terms of developing treatments to manage symptoms and improve the quality of life for children with catastrophic neurologic diseases, while the underlying genetic causes of these serious and progressive diseases often remain incompletely understood and are rarely targeted with a drug. My research at St. Jude centers on identifying pediatric neurologic diseases in which there is a high unmet need for targetable treatments, understanding how the associated gene mutations cause disease, and developing a strategy for drug development specific to that child. We are building the infrastructure to perform efficient clinical trials for these novel gene-targeted drugs, with the goal of altering the fundamental cause and course of the disease.

Finkel Research Summary
Many catastrophic pediatric neurologic diseases have a genetic mutation component underpinning the disease. My research, as well as the greater work of the Center for Experimental Neurotherapeutics (CENT) within the Pediatric Translational Neuroscience Initiative (PTNI), aims to understand these underpinnings by identifying and targeting areas of pediatric neurology with high unmet need, where the genes have been identified, the disease mechanism is known and we have an understanding of the disease’s natural history. Pharmaceutical companies may not have a commercial interest in pursuing treatments for many of these neurogenetic diseases, due to small patient population sizes; however, because of the aggressive and progressive nature of these diseases, finding better, targetable treatments is an imperative and is critical to the St. Jude mission.
My research is focused on genetic diseases that affect neuromuscular function, such as spinal muscular atrophy (SMA), muscular dystrophies, and a collection of inherited neuropathies called Charcot-Marie-Tooth disease. SMA is a rare genetic condition that causes progressive muscle weakness, which, when untreated, prevents infants with the most severe form from gaining motor development and often leads to early mortality. One noteworthy approach my colleagues and I have pursued in addressing this disease is the drug risdiplam, which slows muscular atrophy progression. This Food and Drug Administration (FDA)–approved drug was previously approved for children 2 months and older; however, our research demonstrated that early intervention with this drug before symptoms arise, even in newborn babies, is safe and effective. This research has led to a change in FDA approval, allowing it to be used in treating younger patients, and has laid the groundwork for future research into early interventions for neurogenetic diseases. This work also led to St. Jude’s pioneering work in prenatal SMA treatment with risdiplam, which showed promise in a first-of-its-kind study in 2025.
While my research, and CENT and PTNI on a larger scale, largely focuses on gene-targeted treatments at the DNA or RNA level, it is important to recognize that, in some cases, small-molecule drugs that target downstream pathways can also prove effective in tempering the ravages of some of these neurogenetic diseases. In selected cases, we engage in clinical trials of these downstream modifiers.
Within St. Jude, I collaborate closely with my colleagues to address neuromuscular dysfunction and other catastrophic pediatric neurological diseases. Among my collaborators are Andrea Gropman, MD, whose work focuses on neurometabolic disorders; Heather Mefford, MD, PhD, and her research exploring genes that cause early onset epilepsy and developmental disorders; Peter McKinnon, PhD, whose research has contributed significantly to neurological conditions including ataxia-telangiectasia (A-T); Joshua Burns, PhD, whose work assesses motor functions of patients with neuromuscular diseases, among other gait disturbances; and my other fellow PTNI leaders. Our multidisciplinary approach to these neurological diseases has allowed us to make headway in drastically improving the lives of our patients.
Selected Publications
About Richard Finkel, MD

Richard Finkel, MD, is the Director of CENT within PTNI and a member of the Department of Genomic & Translational Neuroscience. He joined St. Jude in 2020 to develop clinical applications for therapeutic findings within PTNI.
Finkel earned his bachelor's degree from Washington & Jefferson College, Washington, Pennsylvania. He then earned his Doctor of Medicine from Washington University, St. Louis, Missouri. He completed a pediatrics internship and residency, followed by a neurology residency, at Boston Children's Hospital, Harvard Medical School, Boston, Massachusetts. He also completed a neuromuscular fellowship while at Harvard Medical School.
While his work developing treatments for catastrophic neurologic diseases, including SMA, is notable, Finkel has also distinguished himself as an enthusiastic collaborator among his peers. In 2025, he was elected as a Member of the Association of American Physicians in recognition of his valuable contributions to medicine and his commitment to fostering innovation and collaboration among physician scientists.
Contact us
Richard S. Finkel, MD
Department of Genomic & Translational Neuroscience
Center for Experimental Neurotherapeutics
MS 760
St. Jude Children’s Research Hospital

Memphis, TN, 38105-3678 USA GET DIRECTIONS